Life-Sustaining Treatment Patients Endure Up to 12.7 Times the Maximum Pain of a Single Disease... First Revealed by Bank of Korea and NHIS
by Kim Yuri
Published 11 Dec.2025 14:00(KST)
Updated 11 Dec.2025 14:50(KST)
Top 20% Score 127 on Pain Index... Up to 12.7 Times the Maximum Pain of a Single Disease or Procedure
Despite 84% Refusal Intent, Only 17% Actually Withdrawn... "Time for Social Consensus on Systemic Limitations"
'Personalized' Advance Directive
When the suffering experienced by patients undergoing life-sustaining treatment was calculated for the first time in the world, it was found to reach up to 12.7 times the extreme pain of trigeminal neuralgia. While 84.1% of people aged 65 or older expressed their intention not to receive life-sustaining treatment if there was no chance of recovery, in reality, only 16.7% of actual deaths involved withholding or discontinuing life-sustaining treatment.
The Bank of Korea and the National Health Insurance Service, through joint research, agreed that it is time to address the limitations of the life-sustaining treatment decision system so that patients' wishes can be more fully respected in clinical practice. To this end, they emphasized the need to collect more personalized advance directives for life-sustaining treatment to strengthen patient autonomy, and to resolve both institutional blind spots and issues regarding the timing of implementation. Ensuring continuity of care was also highlighted as essential.
Lee Inro, Deputy Director of the Population and Labor Research Division at the Bank of Korea’s Economic Research Institute, stated this during a joint symposium with the National Health Insurance Service held at the Bank of Korea in Jung-gu, Seoul, on the 11th, as he presented the joint research, "Life-Sustaining Treatment: Whose Choice Is It? The Gap Between Patient Preferences and Medical Reality, and Suggestions for Improvement" (Kim Taekyung, Lee Inro, Jeong Jongwoo, Yoo Inkyung, Han Eunjeong, Park Youngwoo).
“Focusing on Patient Suffering” - Top 20% Score 127.2... Up to 12.7 Times the Maximum Pain of a Single Disease or Procedure
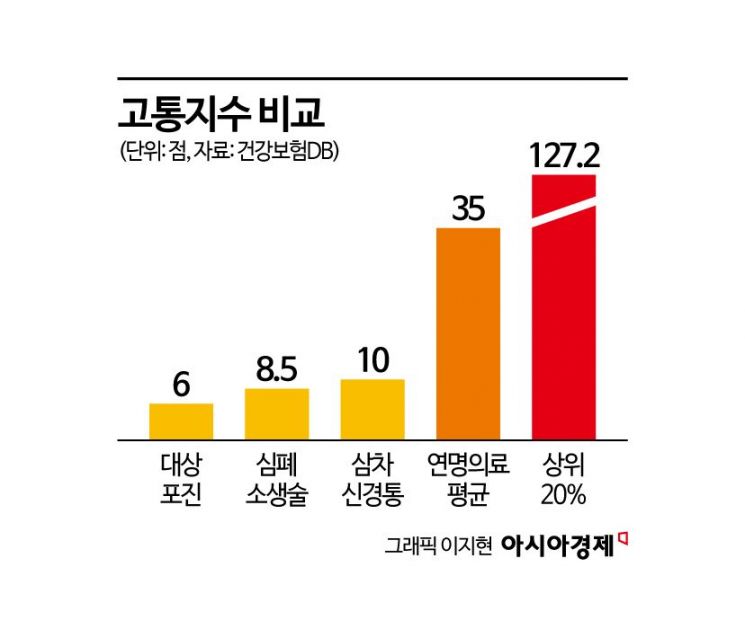
According to the "Life-Sustaining Treatment Suffering Index," calculated for the first time in the world in this study, the average physical suffering score for patients receiving life-sustaining treatment was 35. This is about 3.5 times the maximum pain experienced in a single disease or procedure, such as shingles (6 points), cardiopulmonary resuscitation (8.5 points), or trigeminal neuralgia (10 points). For patients in the top 20% of the index, the suffering score reached 127.2, which is approximately 12.7 times higher.
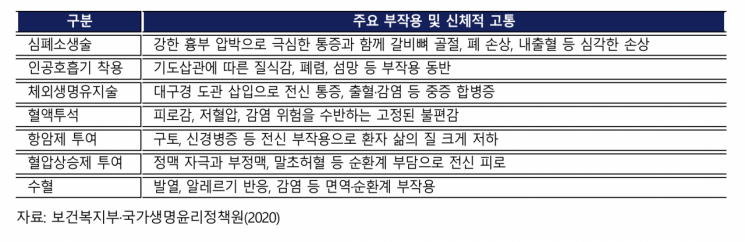
The Life-Sustaining Treatment Suffering Index was designed to simultaneously reflect the intensity and frequency of procedures specified by the Life-Sustaining Treatment Decision Act, such as cardiopulmonary resuscitation, hemodialysis, chemotherapy, mechanical ventilation, extracorporeal life support, blood transfusion, and vasopressors. By weighting the intensity of pain for each procedure with its frequency, a comprehensive index of the total physical suffering actually experienced by patients was calculated. Lee explained, "Since patients eligible for life-sustaining treatment are unable to respond, we conservatively estimated suffering based on responses from patients who recovered after undergoing these procedures," adding, "These results show that certain patient groups subjected to intensive high-intensity procedures bear extremely severe physical burdens."
A significant gap was also found between patient preferences and medical reality. While 84.1% of elderly people aged 65 or older expressed their intention to refuse life-sustaining treatment when there was no chance of recovery, only 16.7% of actual deaths among this age group involved withholding or discontinuing such treatment. Lee noted, "This suggests that a considerable number of elderly patients undergo life-sustaining procedures until just before death, regardless of their own wishes."
The number of patients receiving life-sustaining treatment increased rapidly by an average of 6.4% per year from 2013 to 2023. In addition to the trend factor of population aging (which contributed about 60%), the research team analyzed that a combination of institutional and structural factors restricting patient autonomy throughout the entire process-from advance discussions, choice of medical institution, end-of-life determination, to post-discontinuation care-also played a role.
Lee explained, "A culture that avoids discussions about death leads to a passive attitude toward documenting end-of-life treatment preferences in advance, and the current advance directive for life-sustaining treatment is structured so that patients must make an all-or-nothing choice about discontinuation, making it difficult to reflect individual values and preferences for specific procedures." He also pointed out, "At the stage of choosing a medical institution, it is difficult to access the 'Medical Institution Ethics Committee' or 'Public Ethics Committee' required for discontinuing life-sustaining treatment, which is another limitation."
Additional issues identified include the difficulty of determining the "end-of-life phase," which is defined under current law as a "state where recovery is impossible and death is imminent," and the lack of care infrastructure after discontinuation of life-sustaining treatment. Lee stated, "Looking at cases where life-sustaining treatment was discontinued within one month before death, about 40% made the decision to discontinue only within the final week," adding, "These patients underwent an average of 6.8 life-sustaining procedures during that month."
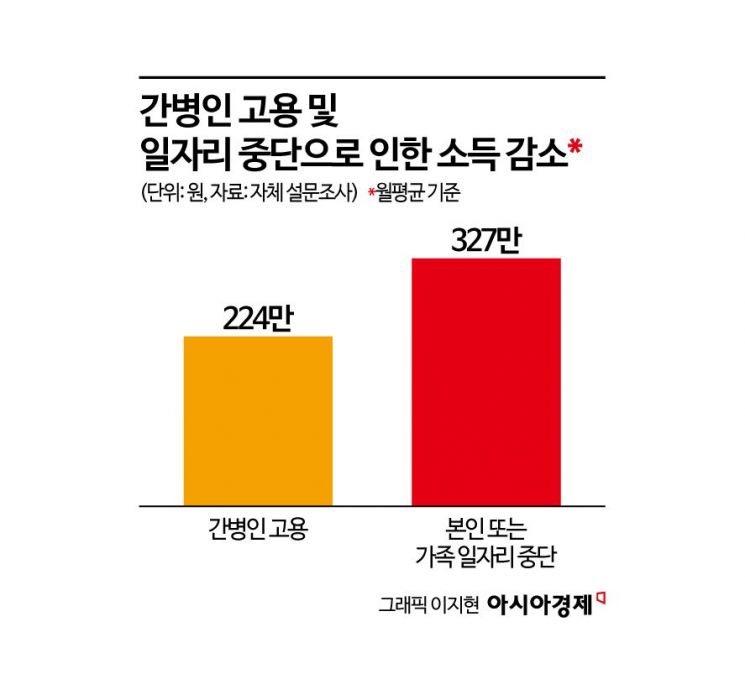
In addition to patient suffering, the increasing economic burden on families was also cited as a social issue. The average end-of-life medical expenses per patient (excluding health insurance coverage, i.e., out-of-pocket expenses for the year prior to death) increased from 5.47 million won in 2013 to 10.88 million won in 2023, rising by an average of 7.2% per year-about double. This is equivalent to 40% of the median income of households aged 65 or older. Patient families may also face additional economic burdens such as hiring caregivers or taking leave or resigning from work.
The research team projected that if the current rate of nearly 70% of elderly deaths involving life-sustaining procedures continues, National Health Insurance spending on life-sustaining treatment will rise from 3 trillion won in 2030 to 16.9 trillion won in 2070. In contrast, if the rate drops to 15% in line with survey results, the cost would be about 3.6 trillion won. Lee stated, "If the saved costs are reallocated to hospice and other care facilities, the quality of end-of-life care for patients could be greatly improved."
Detailed Recording of Personal Preferences, More Items Needed in Advance Directives
The research team emphasized the need to introduce a more personalized form of advance directive for life-sustaining treatment to more accurately reflect patients' specific preferences and values in clinical settings. The new form would include: ▲selective refusal of legally defined life-sustaining procedures; ▲decisions regarding artificial nutrition, which is not currently included in legal life-sustaining treatment but closely related to sustaining life; ▲organ donation intentions; and ▲designation of a healthcare proxy. Lee explained, "We designed the form to include a free-writing section for wishes such as place of death and type of care, so patients can contemplate and record their preferences for the end-of-life process in detail in advance." He added, "However, since issues like organ donation and discontinuation of artificial nutrition may require further social discussion, we hope to first gradually reflect the legally defined procedure-specific choices in the current form."
It was also analyzed that institutional and financial support should be strengthened so that patients can fully exercise their autonomy in all medical institutions, including small and medium-sized hospitals and long-term care hospitals. Lee stated, "To protect patients who become unable to express their wishes without having completed an advance directive, discussions should also be held on introducing a 'healthcare proxy system' that allows patients to designate a trusted person in advance." He emphasized, "As the life-sustaining treatment decision system is gradually taking root, it is also time to begin social discussions on whether to adjust the timing of discontinuation, which is currently limited to the 'end-of-life phase.'"
Lee concluded, "The goal of improving the life-sustaining treatment system is not to simply reduce the use of life-sustaining treatment itself, but to help individuals fully contemplate how they wish to conclude their lives in accordance with their own values, and to ensure that their self-determination is respected until the very end." He added, "Future discussions on life-sustaining treatment should focus on achieving social consensus on how to harmonize respect for self-determination with the value of respect for life. Addressing end-of-life medical issues for patients currently left in the blind spots of the system will also be an important task for future discussions."
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.